[ad_1]
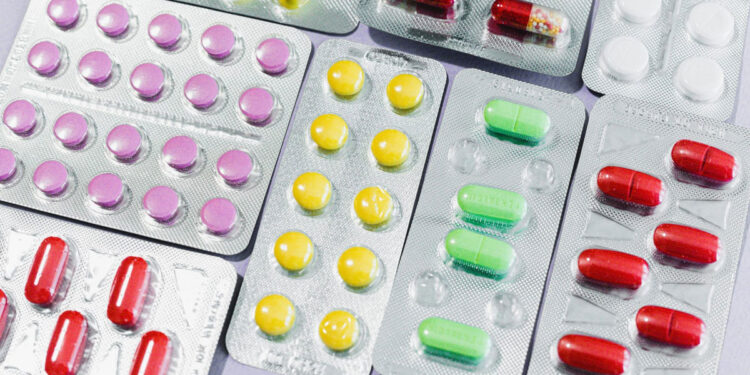
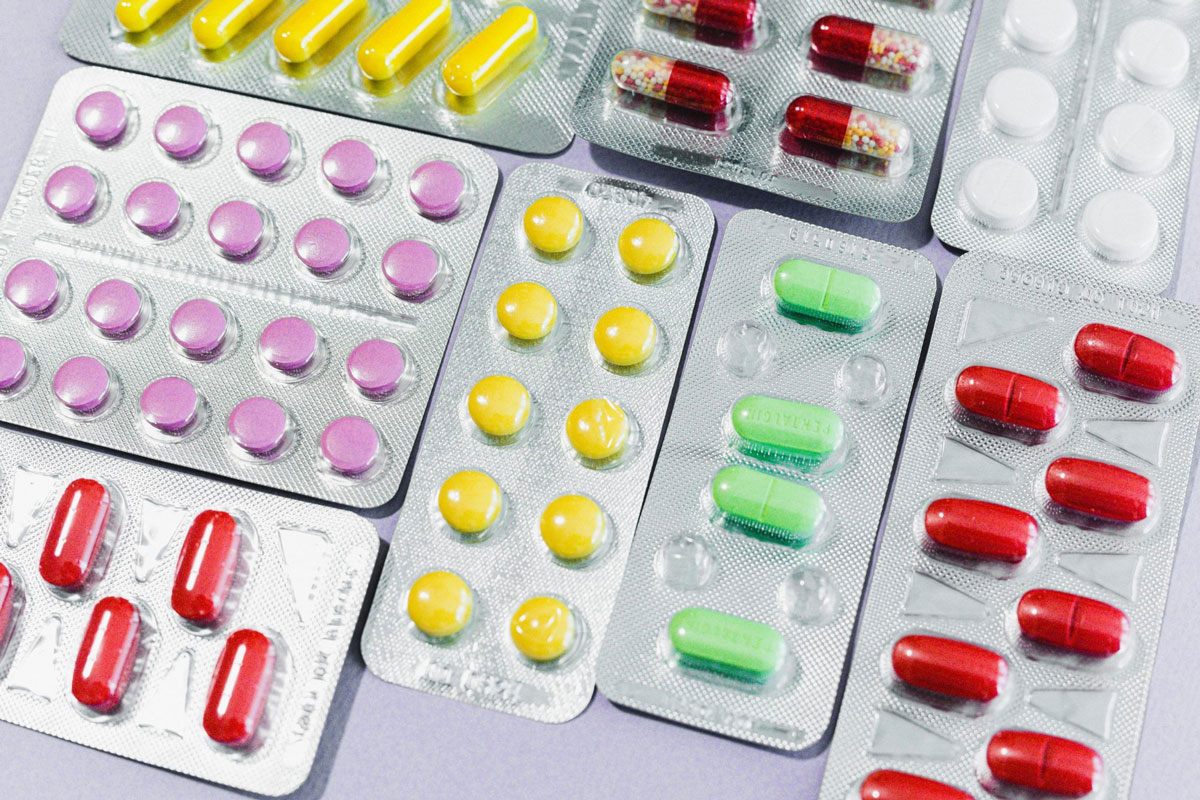 SPRINGFIELD – When a woman requires a hysterectomy, the surgical removal of her uterus, ovaries and fallopian tubes causes estrogen to drop and menopause to begin. Insurance companies will soon be required to cover hormone therapy treatments under a plan led by State Senator Linda Holmes.
SPRINGFIELD – When a woman requires a hysterectomy, the surgical removal of her uterus, ovaries and fallopian tubes causes estrogen to drop and menopause to begin. Insurance companies will soon be required to cover hormone therapy treatments under a plan led by State Senator Linda Holmes.
“A lack of estrogen causes women to develop osteoporosis, weak bones, hot flashes and other symptoms,” Holmes (D-Aurora) said. “Hormone therapy replaces some or all of the estrogen the woman’s ovaries would be making. Adding estrogen back into a woman’s body lowers their risk of certain medical conditions.”
Holmes’ new law requires insurance companies to cover the costs associated with medically necessary hormone therapy who have induced menopause for patients who undergo a hysterectomy. It applies to all plans issued or renewed on or after Jan. 1, 2024 that are commercial group or individual health plans regulated under the Insurance Code, as well as state employee plans, Medicaid plans, HMO plans and plans administered under Municipal Code, Counties Code, School Code, the Limited Health Service Organization Act and the Voluntary Health Services Plans Act.
“Hot flashes, weak bones and osteoporosis greatly lessen the quality of life for women who suffer from the loss of estrogen due to menopause,” Holmes said. “There’s no reason they must suffer when there is an effective course of treatment, and it will be more readily affordable and accessible under this new plan.”
Rep. Keith Wheeler (R-North Aurora, 50th District) is the House sponsor of the bill; he recognizes women who must have a hysterectomy need the assistance for their bodies to re-regulate the many side effects of losing estrogen, and the peace of having the treatment covered by their insurance.
HB5254 was signed into law Friday and takes effect January 1, 2023.
[ad_2]
Source link