[ad_1]
Following the Supreme Court’s overturning of Roe v. Wade last week, Americans who live in areas that ban abortion now must travel out-of-state in order to receive the medical care they’re seeking.
On top of the financial burden created by travel alone, abortions can cost anywhere from $350 to over $1,500. But depending on the state you live in and your insurance provider, health insurance can cover some or all of the bill.
Insider spoke with two health policy experts about which insurance plans cover abortion, and questions to ask your provider in the post-Roe era.
Which types of insurance plans cover abortion?
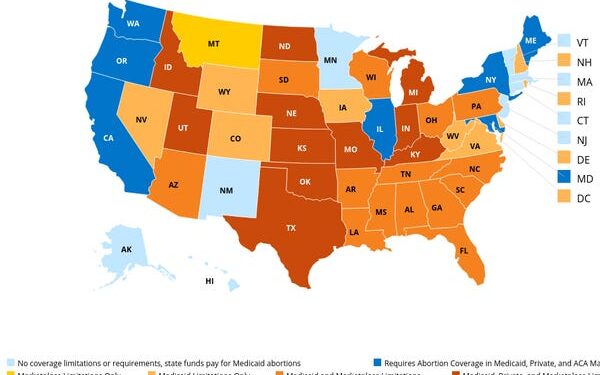
KFF
After the fall of Roe v. Wade, many companies across the US announced they would cover travel costs for employees seeking out-of-state medical care.
Employer health insurance falls into two categories: fully-insured plans and self-insured plans. A fully-insured plan is when an employer purchases health coverage from a state-regulated insurance company.
By comparison, companies with self-insured plans pay for employees’ medical bills directly. Approximately 64% of US workers were covered by self-funded health insurance plans in 2021, according to Statista.
State laws — including those that outlaw insurance providers from covering abortions — can only regulate fully-insured plans. Companies with self-insured plans are “free to make whatever coverage decisions they want,” Sara Rosenbaum J.D., a professor and founding chair of health law and policy at George Washington University’s school of public health, told Insider.
“The woman may have to travel and [the provider] would have to make clear that that they’ll let you go out of network for the care,” she said. “But they could certainly cover it.”
Currently, only eleven US states have laws that prohibit abortion coverage from being included in fully-funded private insurance policies, according to health policy nonprofit KFF.
“So there are some states that will ban abortion, but that have not banned coverage,” Laurie Sobel, the Associate Director for Women’s Health Policy at KFF, told Insider, adding that it’s “probably a matter of time” before those states ban insurance coverage as well.
When it comes to federally-funded health insurance, coverage is only offered in very specific cases. Due to the Hyde amendment, federal funds can’t be used to pay for abortions. That means Medicaid is unable to cover abortions unless the pregnancy is life-threatening or resulted from rape or incest.
Questions to ask your employer or insurance provider in the post-Roe era
While employers have largely focused on travel costs in their corporate responses to the fall of Roe v Wade, there are other logistical hurdles companies need to consider in order to ensure their employees have access to out-of-state care, Sobel told Insider.
“It’s important to look at the structure of the plan. So what is the deductible? What is the copay? What is the network?” she said. “If abortion is now illegal in the state that you reside in, then there needs to be some contract with the clinic out of state.”
If the out-of-state abortion provider is not in-network, the deductible could be more expensive than the procedure itself, she explained.
“Even employers who have the best of intentions and are trying to cover this, it will be challenging just to make it actually work in a way that the person doesn’t have to pay out of pocket,” Sobel added. “For many workers, paying out of pocket won’t be financially feasible.”
Here are five questions Sobel recommends asking your employer or insurance provider in order to determine the extent of your plan’s abortion coverage:
1. Is abortion covered?
2. Are there any restrictions?
3. Does the deductible apply?
4. Is there cost sharing?
5. Are there out-of-state abortion providers in network?
[ad_2]
Source link